Predictive Factors of Dysmenorrhea Among Women of Reproductive Age: A Multivariate Logistic Regression Analysis of Lifestyle and Biological Determinants
Keywords:
Dysmenorrhea, Sleep Quality, Medication Use, Logistic RegressionAbstract
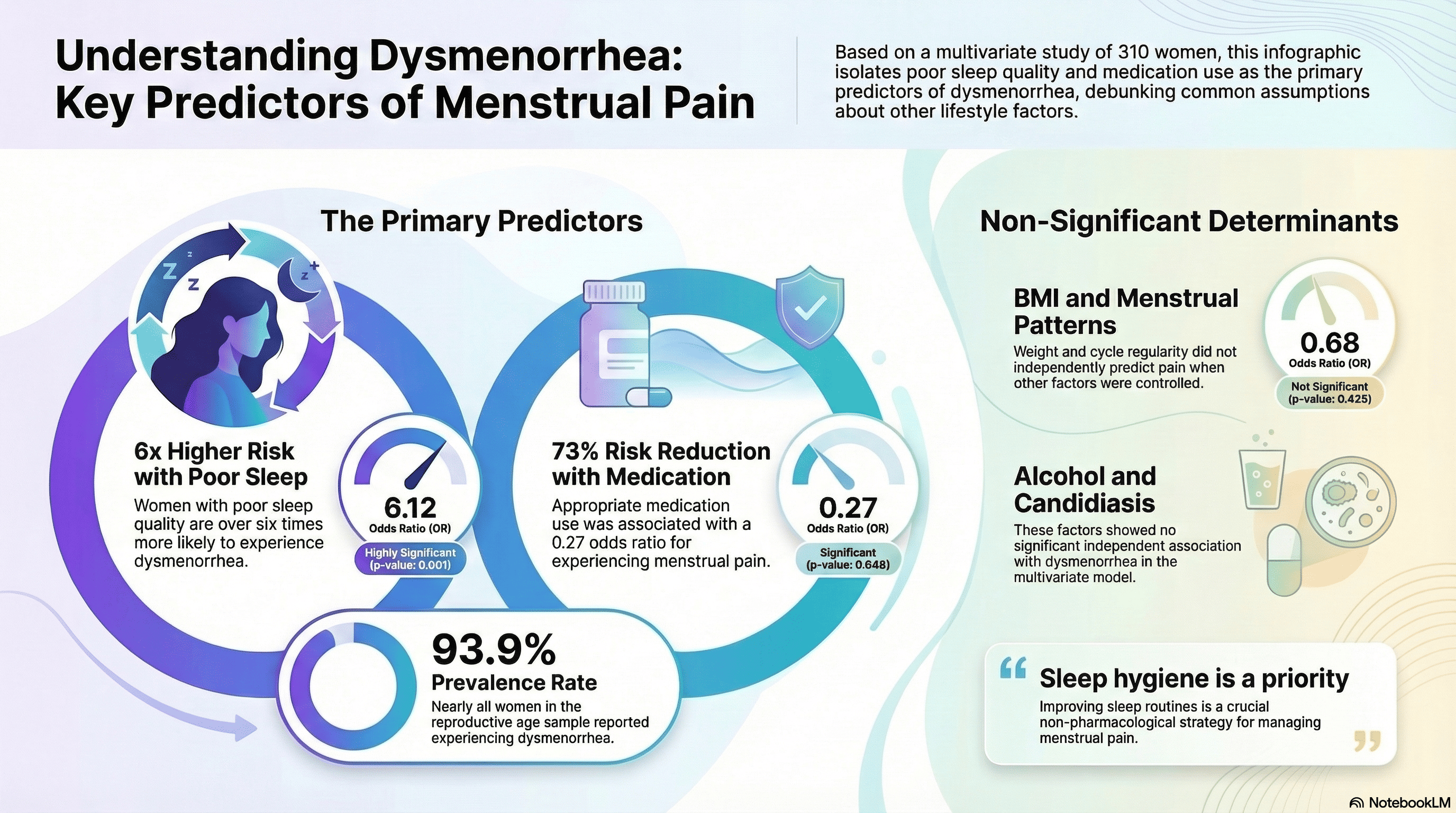
Dysmenorrhea is a prevalent gynecological condition that adversely affects women’s daily functioning and quality of life. This cross-sectional study examined associations between lifestyle and biological factors and dysmenorrhea among 310 women of reproductive age recruited from community settings in Padang, West Sumatra, Indonesia. Data on menstrual patterns, history of candidiasis, alcohol consumption, medication use, sleep quality, and body mass index (BMI) were collected using structured questionnaires and anthropometric measurements. In bivariate analysis, candidiasis and alcohol consumption were associated with dysmenorrhea; however, these associations were attenuated and did not remain statistically significant in the adjusted multivariate model. Multivariate logistic regression identified two independent associations, poor sleep quality was associated with increased odds of dysmenorrhea (OR = 6.12, 95% CI: 2.07–18.08, p = 0.001), while medication use was associated with decreased odds of dysmenorrhea (OR = 0.27, 95% CI: 0.08–0.99, p = 0.048). These findings indicate that, after adjustment for other factors, sleep quality and use of medication were the primary correlates of dysmenorrhea in this sample. Interventions that promote sleep hygiene and ensure appropriate symptom management may help reduce the burden of dysmenorrhea.
Downloads
References
MacGregor B, Allaire C, Bedaiwy MA, Yong PJ, Bougie O. Disease burden of dysmenorrhea: Impact on life course potential. Int J Womens Health. 2023;499–509.
Núñez-Troconis J, Carvallo D, Martínez-Núñez E. Primary Dysmenorrhea: pathophysiology. Invest Clin. 2021;4:378–406.
Maity S, Wray J, Coffin T, Nath R, Nauhria S, Sah R, et al. Academic and social impact of menstrual disturbances in female medical students: a systematic review and meta-analysis. Front Med. 2022;9:821908.
Francavilla R, Petraroli M, Messina G, Stanyevic B, Bellani AM, Esposito SMR, et al. Dysmenorrhea: epidemiology, causes and current state of the art for treatment. Clin Exp Obstet Gynecol. 2023;50(12):274.
Çinar GN, Akbayrak T, Gürşen C, Baran E, Üzelpasacı E, Nakip G, et al. Factors related to primary dysmenorrhea in Turkish women: a multiple multinomial logistic regression analysis. Reprod Sci. 2021;28(2):381–92.
Rugvedh P, Gundreddy P, Wandile B. The menstrual cycle’s influence on sleep duration and cardiovascular health: a comprehensive review. Cureus. 2023;15(10).
Cao M, Ye F, Xie W, Yan X, Ho M, Cheung DST, et al. Effectiveness of auricular acupoint therapy targeting menstrual pain for primary dysmenorrhea: A systematic review and meta‐analysis of randomized controlled trials. Worldviews Evidence‐Based Nurs. 2023;20(6):621–33.
Bala R, Singh V, Rajender S, Singh K. Environment, lifestyle, and female infertility. Reprod Sci. 2021;28(3):617–38.
Reichert D, Brüßler S, Reichert M, Ebner-Priemer U. Understanding alcohol consumption and its antecedents and consequences in daily life: the why and the how. In Springer; 2024.
Shroff S. Infectious vaginitis, cervicitis, and pelvic inflammatory disease. Med Clin. 2023;107(2):299–315.
Lennon O, Hall P, Blake C. Predictors of adherence to lifestyle recommendations in stroke secondary prevention. Int J Environ Res Public Health. 2021;18(9):4666.
Mammo M, Alemayehu M, Ambaw G. Prevalence of primary dysmenorrhea, its intensity and associated factors among female students at high schools of Wolaita Zone, Southern Ethiopia: cross-sectional study design. Int J Womens Health. 2022;1569–77.
Wang YL, Zhu HL. The prevalence and associated risk factors of primary dysmenorrhea among women in Beijing: a cross-sectional study. Sci Rep. 2025;15(1):5003.
Watanabe M, Balena A, Tuccinardi D, Tozzi R, Risi R, Masi D, et al. Central obesity, smoking habit, and hypertension are associated with lower antibody titres in response to COVID‐19 mRNA vaccine. Diabetes Metab Res Rev. 2022;38(1):e3465.
Chung WK, Brothers K, Bradbury A, Chanprasert S, Orlando L, Torkamani A, et al. Genomic medicine implementation protocols in the PhenX Toolkit: tools for standardized data collection. Genet Med. 2021;23(9):1783–8.
Kalnins A, Praitis Hill K. The VIF score. What is it good for? Absolutely nothing. Organ Res methods. 2025;28(1):58–75.
Carrington AM, Manuel DG, Fieguth PW, Ramsay T, Osmani V, Wernly B, et al. Deep ROC analysis and AUC as balanced average accuracy, for improved classifier selection, audit and explanation. IEEE Trans Pattern Anal Mach Intell. 2022;45(1):329–41.
Fu Y, Wang X, Yang X, Zhao R. Analysis of dysmenorrhea-related factors in adenomyosis and development of a risk prediction model. Arch Gynecol Obstet. 2025;1–9.
saleh Isyaku A, Dakingari AI. " Public Health Perspectives on Dysmenorrhoea: Management, Contributing Factors, and Preventive Strategies. J Med Dent Sci Res. 2025;12(6):19–28.
Chandel S, Das S, Ojha S, Pandey M. Hormonal imbalances and genetic factors in menstrual cycle irregularities. In: Women’s Health: A Comprehensive Guide to Common Health Issues in Women. Bentham Science Publishers; 2024. p. 101–28.
Workowski KA. Sexually transmitted infections treatment guidelines, 2021. MMWR Recomm Reports. 2021;70.
Mote D, Dukle A, Chaudhari N, Maurya MN. A Prospective, Open-label Non-Randomized Clinical Trial to evaluate the Safety and Efficacy of M2-Tone Tablet in Treatment of Dysmenorrhea. J Ayurveda Integr Med Sci. 2025;10(6):4–12.
Zhu M, Huang H. The underlying mechanisms of sleep deprivation exacerbating neuropathic pain. Nat Sci Sleep. 2023;579–91.
Irwin MR, Straub RH, Smith MT. Heat of the night: sleep disturbance activates inflammatory mechanisms and induces pain in rheumatoid arthritis. Nat Rev Rheumatol. 2023;19(9):545–59.
Published
How to Cite
Issue
Section
Copyright (c) 2026 Sunesni Sunesni, Dian Furwasyih, Gina Muthia, Yulia Arifin

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.





















