Factors Associated with Blood Pressure and Cholesterol Level in Adolescents: A Survey Study in An Islamic School in Palu City, Indonesia
Keywords:
Adolescents, Blood pressure, Cholesterol, Natrium, SurveyAbstract
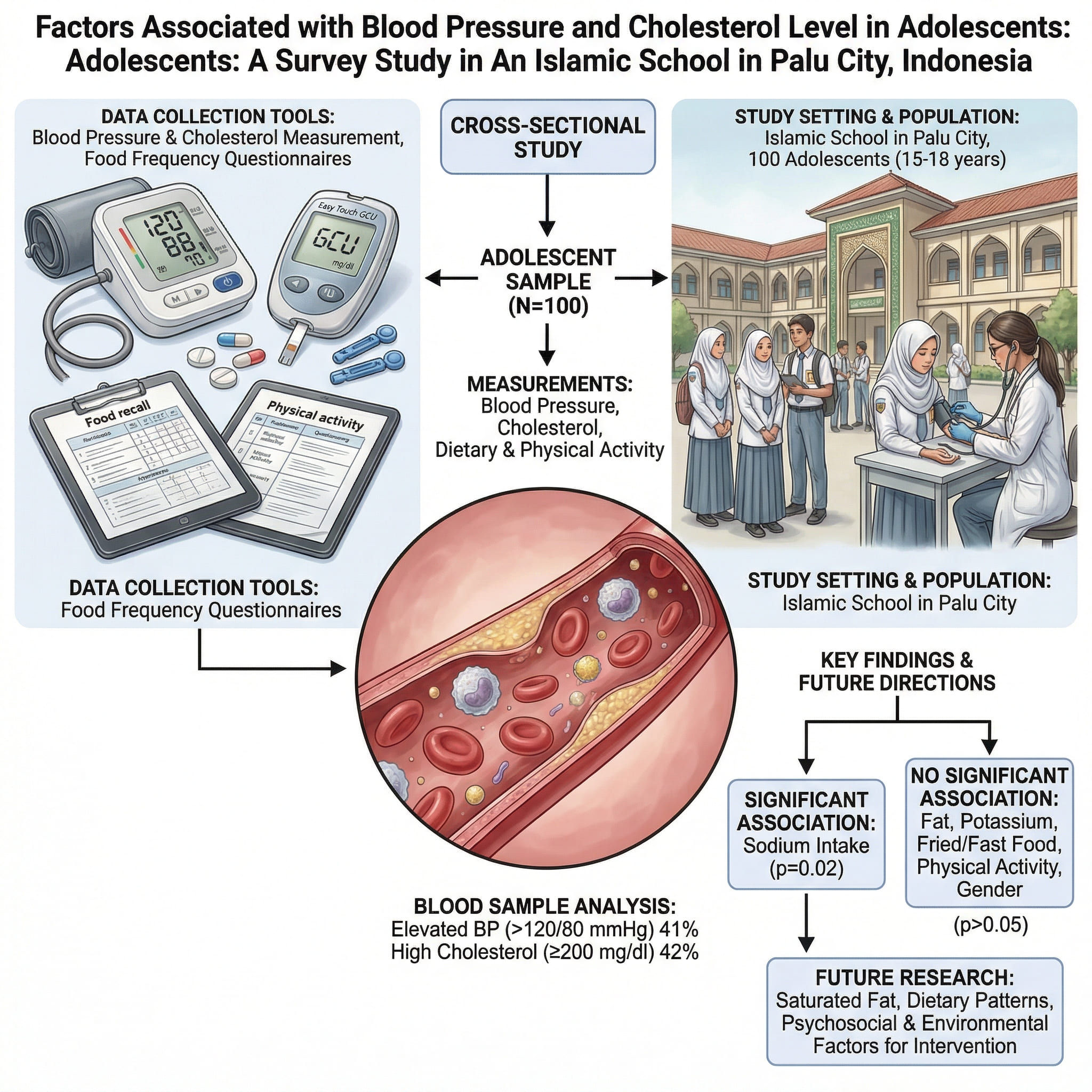
The risk of degenerative diseases, including high blood pressure and high cholesterol levels, can occur at any age. This study aims to explore the relationship between several modifiable factors and blood pressure and cholesterol levels in adolescents. The survey was conducted in one of the Islamic schools in a densely populated area in Palu City using a cross-sectional study design with a simple random sampling technique on 100 respondents aged 15–18 years. Dietary and habitual intake as well as physical activity were collected through a 2x24-hour food recall questionnaire, a qualitative food frequency questionnaire, and an IPAQ questionnaire. Blood pressure and blood cholesterol levels were measured using a digital tension meter and easy touch GCU, respectively. Results indicated that 41 percent of adolescents had elevated blood pressure (>120/80 mmHg) and 42 percent had high cholesterol levels (≥200 mg/dl), with an average systolic blood pressure of 121 mmHg and cholesterol levels of 199 mg/dL. Only sodium was significantly associated with blood pressure (p = 0.02), and no factors were significantly associated with cholesterol levels after multivariate analysis by including other variables: fat intake, potassium intake, fried and fast-food eating habits, physical activity, and gender (p > 0.05). Further exploration should include additional dietary factors such as saturated fat intake and overall dietary patterns, as well as psychosocial, and environmental influences to help design appropriate nutritional behavior change interventions for adolescents.
Downloads
References
Norris SA, Frongillo EA, Black MM, Dong Y, Fall C, Lampl M, et al. Nutrition in adolescent growth and development. The Lancet. 2022 Jan 8;399(10320):172–84.
Moore Heslin A, McNulty B. Adolescent nutrition and health: characteristics, risk factors and opportunities of an overlooked life stage. Proceedings of the Nutrition Society. 2023/03/16 ed. 2023;82(2):142–56.
Dewi NU, Krisnasari S, Sanjaya K, Aida N. Dietary Quality and Nutritional Status of Adolescents in Rural Areas of Sigi Regency, Indonesia. Media Gizi Indonesia. 2025;20(2):178–84.
Dewi NU, Khomsan A, Dwiriani CM, Riyadi H, Ekayanti I, Hartini DA, et al. Factors Associated with Diet Quality among Adolescents in a Post-Disaster Area: A Cross-Sectional Study in Indonesia. Nutrients. 2023;15(5):1–22.
Health Research and Development Unit. Indonesia Basic Health Research. Jakarta; 2018.
Health Research and Development Unit. Indonesia Basic Health Research. Jakarta; 2013.
Pengpid S, Peltzer K. National high prevalence, and low awareness, treatment and control of dyslipidaemia among people aged 15–69 years in Mongolia in 2019. Scientific Reports. 2022;12(1):10478.
Abujbara M, Batieha A, Khader Y, Jaddou H, El-Khateeb M, Ajlouni K. The Prevalence of Dyslipidemia among Jordanians. Journal of Lipids. 2018 Jan 1;2018(1):6298739.
Gebreegziabiher G, Belachew T, Mehari K, Tamiru D. Prevalence of dyslipidemia and associated risk factors among adult residents of Mekelle City, Northern Ethiopia. PLOS ONE. 2021 Feb 9;16(2):e0243103.
Pan L, Yang Z, Wu Y, Yin RX, Liao Y, Wang J, et al. The prevalence, awareness, treatment and control of dyslipidemia among adults in China. Atherosclerosis. 2016 May 1;248:2–9.
Suciawati A, Silawati V, Mulyati D. Factors Associated with Cholesterol Levels among Adolescent Girls. Jurnal Ilmiah Kebidanan Indonesia. 2019;15:30–6.
Sari HP, Fadlilah SH, Febriani AR, Yasmin A, Fadilah FN, Azizah NF. The Influence of Physical Activity, Fast Food, and Body Composition on Hypercholesterolemia in Young Adults: A Step Toward SDGs - Good Health and Well-being. E3S Web of Conferences. 2025;609.
World Health Organization. Global report on hypertension: the race against a silent killer. Vol. 01. Geneva; 2023. 1–7 p.
Ministry of Health of The Republic of Indonesia. Indonesian Health Survey 2023. Jakarta; 2023.
Sudikno S, Mubasyiroh R, Rachmalina R, Arfines PP, Puspita T. Prevalence and associated factors for prehypertension and hypertension among Indonesian adolescents: a cross-sectional community survey. BMJ Open. 2023 Mar 1;13(3):e065056.
Budreviciute A, Damiati S, Sabir DK, Onder K, Schuller-Goetzburg P, Plakys G, et al. Management and Prevention Strategies for Non-communicable Diseases (NCDs) and Their Risk Factors. Frontiers in public health. 2020;8:574111.
Zhu Y, Wang Z. Association between joint physical activity and healthy dietary patterns and hypertension in US adults: cross-sectional NHANES study. BMC Public Health. 2024;24(1):855.
Ghodeshwar GK, Dube A, Khobragade D. Impact of Lifestyle Modifications on Cardiovascular Health: A Narrative Review. Cureus. 2023 July;15(7):e42616.
Te Morenga L, Montez JM. Health effects of saturated and trans-fatty acid intake in children and adolescents: Systematic review and meta-analysis. PLOS ONE. 2017 Nov 17;12(11):e0186672.
Gadiraju T V, Patel Y, Gaziano JM, Djoussé L. Fried Food Consumption and Cardiovascular Health: A Review of Current Evidence. Nutrients. 2015 Oct;7(10):8424–30.
Kim BS, Yu MY, Shin J. Effect of low sodium and high potassium diet on lowering blood pressure and cardiovascular events. Clinical hypertension. 2024 Jan;30(1):2.
Estrada CAM, Lomboy MFTC, Gregorio ER, Amalia E, Leynes CR, Quizon RR, et al. Religious education can contribute to adolescent mental health in school settings. International Journal of Mental Health Systems. 2019;13(1):28.
Rimbawan R, Nurdiani R, Rachman PH, Kawamata Y, Nozawa Y. School Lunch Programs and Nutritional Education Improve Knowledge, Attitudes, and Practices and Reduce the Prevalence of Anemia: A Pre-Post Intervention Study in an Indonesian Islamic Boarding School. Nutrients. 2023 Feb;15(4).
Solihin I, Hasanah A, Fajrussalam H. Core Ethical Values of Character Education Based on Islamic Values in Islamic Boarding Schools. International Journal on Advanced Science, Education, and Religion. 2020;3(2):21–33.
Keleher A, Neggaz M, Cliff CM, Muhammad YI, Mathews A, Quadri H, et al. Incorporating Halal Into Healthy and Equitable Dietary Patterns to Address Food and Nutrition Security Among K-12 and University Students: A Perspective. Journal of Nutrition Education and Behavior. 2024;56(9):663–71.
Elgharbawy A, Azmi NAN. Food as medicine: How Eating Halal and Tayyib Contributes to a Balanced Lifestyle. Halalsphere. 2022;2(1):86–97.
Briawan D, Khomsan A, Alfiah E, Nasution Z, Putri PA. Preference for and consumption of traditional and fast foods among adolescents in Indonesia. Food Research. 2023;7(4):211–26.
Pakpahan C, Amanda B, Sumino R, Azlansyah A, Simatupang CM, Handini LP, et al. Navigating adolescence matters in Indonesia: insights and needs of students in Islamic schools. The Pan African medical journal. 2025;50:100.
Lemeshow S, Hosmer DW, Klar J, Lwanga SK. Adequacy of Sample Size in Health Studies. Vol. 47, World Health Organization. Geneve; 1990. 347 p.
Ministry of Health of the Republic of Indonesia. Guidelines for Filling Out the Indonesia Health Survey Questionnaire 2023 (Version 11). Jakarta; 2023.
IPAQ Research Committee. Guidelines for Data Processing and Analysis of the International Physical Activity Questionnaire (IPAQ) – Short and Long Forms. 2005.
Almahmoud OH, Arabiat DH, Saleh MY. Systematic review and meta-analysis: Prevalence of hypertension among adolescents in the Arab countries. Journal of pediatric nursing. 2022;65:e72–9.
Liu K, Li C, Gong H, Guo Y, Hou B, Chen L, et al. Prevalence and Risk Factors for Hypertension in Adolescents Aged 12 to 17 Years: A School-Based Study in China. Hypertension. 2021 Nov 1;78(5):1577–85.
Hardy ST, Sakhuja S, Jaeger BC, Urbina EM, Suglia SF, Feig DI, et al. Trends in Blood Pressure and Hypertension Among US Children and Adolescents, 1999-2018. JAMA Network Open. 2021 Apr 1;4(4):e213917–e213917.
Kwok MK, Wong IOL, Schooling CM. Age-period-cohort projection of trends in blood pressure and body mass index in children and adolescents in Hong Kong. BMC Pediatrics. 2020;20(1):1–11.
Gomes ÉIL, Zago VH de S, Faria EC de. Evaluation of Lipid Profiles of Children and Youth from Basic Health Units in Campinas, SP, Brazil: A Cross-Sectional Laboratory Study. Arquivos brasileiros de cardiologia. 2020 Jan;114(1):47–56.
Guirguis-Blake JM, Evans C V, Coppola EL, Redmond N, Perdue LA. Screening for Lipid Disorders in Children and Adolescents: Updated Evidence Report and Systematic Review for the US Preventive Services Task Force. JAMA. 2023 July;330(3):261–74.
Sulistyadewi NPE, Masitah R. Asupan karbohidrat dan lemak dari konsumsi makanan jajanan terhadap status gizi pada remaja. Jurnal Kesehatan Terpadu. 2020;4(2):52–6.
Irwanda M, Suryani D, Krisnasary A. Gambaran Asupan Energi , Zat Gizi Makro Dan Status Gizi Remaja Di SMP N 14 Kota Bengkulu Tahun 2022. AKSARA. 2023;09(January):199–208.
Afifah NN, Hardiansyah A, Darmuin D. Asupan lemak, asupan serat, persepsi body image dan status gizi siswa SMA Kesatrian 1 Semarang. Nutrition Scientific Journal. 2024;3(1):8–18.
Faridi A, Vidyarini A, Prasetya AY. Hubungan Pengetahuan, Kebiasaan Sarapan Dan Asupan Zat Gizi Makro Sarapan Dengan Status Gizi Pada Remaja. Jurnal Riset Gizi. 2023;11(2):106–13.
Sutriani A, Ngadiarti I. ubungan antara asupan energi, protein, lemak, karbohidrat, serat dengan kejadian gizi lebih pada anak remaja usia 1H3-18 tahun di pulau jawa (analisis data sekunder riskesdas 2010). Nutrire Diaita. 2013;5(2):68–80.
Musfira M, Hadju V. Nutrition and Dietary Intake of Adolescent Girls in Indonesia: A Systematic Review. Scripta Medica (Banja Luka). 2024;55(4):473–87.
Song S, Shim JE. Trends in Dietary Intake of Total Fat and Fatty Acids Among Korean Adolescents from 2007 to 2017. Nutrients. 2019 Dec;11(12).
Emamian MH, Ebrahimi H, Hashemi H, Fotouhi A. Salt intake and blood pressure in Iranian children and adolescents: a population-based study. BMC Cardiovascular Disorders. 2021;21(1):1–10.
Brouillard AM, Deych E, Canter C, Rich MW. Trends in Sodium Intake in Children and Adolescents in the US and the Impact of US Department of Agriculture Guidelines: NHANES 2003-2016. The Journal of pediatrics. 2020 Oct;225:117–23.
Ministry of Health of the Republic of Indonesia. Regulation of the Minister of Health of the Republic of Indonesia Number 28 of 2019 concerning Recommended Dietary Allowance (RDA) for the Indonesian People. Jakarta, Indonesia; 2019.
Reddin C, Ferguson J, Murphy R, Clarke A, Judge C, Griffith V, et al. Global mean potassium intake: a systematic review and Bayesian meta-analysis. European journal of nutrition. 2023 Aug;62(5):2027–37.
Farapti F, Maulia PH, Fadilla C, Yogiswara N, Rejeki PS, Miftahussurur M, et al. Community-level dietary intake of sodium, potassium, and sodium-to-potassium ratio as a global public health problem: a systematic review and meta-analysis. F1000Research. 2022;11:953.
Vargas-Meza J, Cervantes-Armenta MA, Campos-Nonato I, Nieto C, Marrón-Ponce JA, Barquera S, et al. Dietary Sodium and Potassium Intake: Data from the Mexican National Health and Nutrition Survey 2016. Nutrients. 2022 Jan;14(2).
Rachmi CN, Jusril H, Ariawan I, Beal T, Sutrisna A. Eating behaviour of Indonesian adolescents: A systematic review of the literature. Public Health Nutrition. 2020;24(Lmic).
Negara BF, Tirtawijaya G, Cho WH, Harwanto D, Sohn JH, Kim JS, et al. Effects of Frying Processes on the Nutritional and Sensory Characteristics of Different Mackerel Products. Vol. 9, Processes. 2021.
Vrevic E, Malovic P, Bacovic D, Bojanic D, Nokic A. Differences in nutritional status and level of physical activity among adolescents living in urban and rural areas of Montenegro - national study. BMC Public Health. 2024;24(1):896.
Nurwanti E, Hadi H, Chang JS, Chao JCJ, Paramashanti BA, Gittelsohn J, et al. Rural–urban differences in dietary behavior and obesity: Results of the riskesdas study in 10–18-year-old Indonesian children and adolescents. Nutrients. 2019;11(11):1–14.
Malik AS, Chatterjee K. A cross-sectional study to compare levels of physical activity among adolescents in rural and urban areas of Western Maharashtra. Medical journal, Armed Forces India. 2023 Dec;79(Suppl 1):S237–43.
Andriyani FD, Biddle SJH, Priambadha AA, Thomas G, De Cocker K. Physical activity and sedentary behaviour of female adolescents in Indonesia: A multi-method study on duration, pattern and context. Journal of Exercise Science & Fitness. 2022;20(2):128–39.
Rifqi MA, Puspikawati SI, Salisa W, Zaman MNU. Sweet Sweetened Beverages Intake and Sedentary Behavior Drive Overweight Trends: A Study of Urban and Rural Adolescents in East Java, Indonesia. Amerta Nutrition. 2025;9(1):34–44.
BPS-Statistics of Palu Municipality. Palu Municipality in Figure 2025. Vol. 25. Palu; 2025.
Ahmad S, Ansari MA, Abedi AJ, Khalil S, Eram U, Khan MNA. Physical Activity Levels and Junk Food Intake among School going Adolescents in a North Indian City. 2023;35(2):182–6.
Popoola AA, Frediani JK, Hartman TJ, Paynabar K. Mitigating underreported error in food frequency questionnaire data using a supervised machine learning method and error adjustment algorithm. BMC Medical Informatics and Decision Making. 2023;23(1):178.
Winpenny EM, van Sluijs EMF, Forouhi NG. How do short-term associations between diet quality and metabolic risk vary with age? European journal of nutrition. 2021 Feb;60(1):517–27.
Filippini T, Malavolti M, Whelton PK, Vinceti M. Sodium Intake and Risk of Hypertension: A Systematic Review and Dose-Response Meta-analysis of Observational Cohort Studies. Current hypertension reports. 2022 May;24(5):133–44.
Polychronopoulou E, Braconnier P, Burnier M. New Insights on the Role of Sodium in the Physiological Regulation of Blood Pressure and Development of Hypertension. Frontiers in cardiovascular medicine. 2019;6:136.
Kazi RN. Silent Effects of High Salt: Risks Beyond Hypertension and Body’s Adaptation to High Salt. Vol. 13, Biomedicines. 2025.
Brady TM, Horst G, Appel LJ, Khoury PR, Urbina EM. Dietary sodium intake and sodium load is associated with arterial stiffness in children and young adults. Journal of hypertension. 2022 Feb;40(2):292–9.
Robinson CH, Chanchlani R. High Blood Pressure in Children and Adolescents: Current Perspectives and Strategies to Improve Future Kidney and Cardiovascular Health. Kidney international reports. 2022 May;7(5):954–70.
Zuin C. Psychosocial factors and hypertension: Exploring the mind-heart connection. J Hypertens Heart Care. 2023;6(3):147.
Johnson SA, Kirkpatrick CF, Miller NH, Carson JAS, Handu D, Moloney L. Saturated Fat Intake and the Prevention and Management of Cardiovascular Disease in Adults: An Academy of Nutrition and Dietetics Evidence-Based Nutrition Practice Guideline. Journal of the Academy of Nutrition and Dietetics. 2023 Dec 1;123(12):1808–30.
de Souza RJ, Mente A, Maroleanu A, Cozma AI, Ha V, Kishibe T, et al. Intake of saturated and trans unsaturated fatty acids and risk of all cause mortality, cardiovascular disease, and type 2 diabetes: systematic review and meta-analysis of observational studies. BMJ (Clinical research ed). 2015 Aug;351:h3978.
Kalwick M, Roth M. A Comprehensive Review of the Genetics of Dyslipidemias and Risk of Atherosclerotic Cardiovascular Disease. Nutrients. 2025 Feb;17(4).
Curtis D. Genetic Variants Associated with Hypertension Risk: Progress and Implications. Pulse (Basel, Switzerland). 2024;12(1):19–26.
Rahfiludin MZ, Asna AF, Suroto, Hidayanti L. Contribution of Snacks and Physical Activities to Elevated Blood Pressure of Adolescent Girls in West Java, Indonesia. Malaysian Journal of Medicine and Health Sciences. 2023;19(4):53–60.
Published
How to Cite
Issue
Section
Copyright (c) 2026 Nikmah Utami Dewi, Disty Rahmawaty Tahir, Ningsih Wulandari

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.





















